Notes on Rotator Cuff Repair
These notes should be read in conjunction with the explanatory notes on shoulder muscle pain. In that booklet, rotator cuff muscle pain was explained and the possibility that the rotator cuff can actually tear.
The rotator cuff is a group of muscle that are responsible for guiding the shoulder and arm. It is really a sheet of muscle and when a part is torn, it must, by necessity, become slightly weaker. The bigger the tear, the more weakness the patient may notice.
Because it is a muscle, it also has the power to strengthen and so the remaining muscle, which is still attached, can get stronger and compensate for the torn part.
Unfortunately, the torn part can never heal itself spontaneously. It does not reattach.
When a patient has a torn rotator cuff, they notice two groups of complaints:
- Pain, which is present on activity during the day and particularly at night.
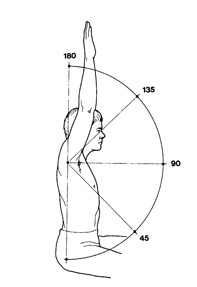
- Weakness. Patients do not have the power to push the arm and hand up into various places. Attempting to do this often provokes extra pain.
In rotator cuff repair surgery, things are very different.
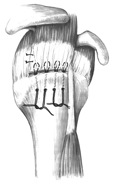
In rotator cuff repair, the surgeon repairs the torn muscle tendon by tacking it back to the bone from which it tore. The tacking stitches are quite weak. The actual glue is made by the body.
This scar glue takes a minimum of six weeks to form so that during that time the patient is not able to use the arm actively at all. This is because the surgeon’s tacking stitches are not strong enough to resist the pull of the muscle. If the patient used the arm, the repair would immediately fail.
This means that every rotator cuff repair patient has to keep his arm in a sling or other immobilisation device, for six weeks. It stays there twenty-four hours a day, except when the patient goes into a shower to wash under the affected arm. He may not use the arm or hand for any activity at all, including cutting food or writing or using a computer keyboard.
During that six weeks, though we need scar to heal the torn muscle, we do not want scar to form in other parts of the shoulder. If it did, then the shoulder would become stiff. To stop this happening, the shoulder has to be moved. The patient is taught to do this himself, with the other arm to do the stretching. This occurs once a day, maintaining the range of movement, preventing glue and scar from forming in the wrong places.
After six weeks, a patient is able to start moving the arm actively for himself, but for six further weeks, only very gently. It therefore takes three months before the scar has matured enough and is safe for normal day to day use. It is only then that one knows that the repair has been a success.
From three months onwards, patients are able to get back to light day-to-day activities but heavy lifting is not allowed for nine months, if at all. The same applies to strenuous activities, such as golf and tennis.
Results:
The results of surgery are proportional to three things: the youth of the patient; the quality of the tendon; and the size of the tear.
Youth of Patient: Younger patients have a higher success rate and better healing than older patients. For rotator cuff tears, ‘young’ is 50, and ‘older’ is over 70. Though the rotator cuff can be repaired in patients over seventy years of age, research shows that the failure rate in this age group is much higher than in patients aged around fifty to sixty years.
Tendon Quality:
If a tear has occurred as a result of sudden trauma, then the repair has a better prognosis. Using the tow rope analogy, if it is a good tow rope but it just pulled something which was much too heavy (a heavy fall), then it is likely to repair quite well. If it is an old, frayed tow rope which failed with relatively little weight, or even spontaneously, then it can easily fail again during the repair process.
Tear Size:
The tear size is measured in centimetres and Mr Kurer will give you a rough idea of the size of your tear. The bigger the tear and the more healing that is required, then the worse the result. Small tears, of say one or two centimetres, tend to heal well whereas bigger tears of four to five centimetres may not heal.
It takes at least nine months before a patient will really know if the operation has been successful, although there will be hints before that. Most of the operations are good for pain relief but success is also measured in terms of restoring power. With a small repair in a young patient then the success rates are approximately 90%. With a large, degenerate tear in a patient around seventy years old, the success rate may be as low as 60%. Patients should think very carefully before embarking on such an involved procedure.
Complications:
Surgery can be complicated in the first instance by infection and though this can be eradicated if picked up quickly, it certainly jeopardises the results of surgery and the repair may well fail altogether, purely because of this. Using keyhole techniques for the repair, infection is very unusual.
Another complication is stiffness. We will work very hard to try and stop stiffness but some people just have an excessive scarring reaction to surgery and become stiff. This too, may jeopardise the repair as it is like trying to drive the car with the handbrake on. This will cause the muscle to tear out.
The third complication is simple repair failure. In a proportion of patients at three to four months, as already outlined, the repair will have failed. The patient will have been through the six weeks of immobilisation and the six weeks of gentle rehabilitation and will not have a successful repair after it. Things can be salvaged with physiotherapy but in certain patients a failure occurs and there is very little that can be done about it. To reiterate, the failure rate is between 10% and 40%, depending on the factors already raised.
 These notes should be read in conjunction with the explanatory notes on shoulder muscle pain. In that booklet, rotator cuff muscle pain was explained and the possibility that the rotator cuff can actually tear.
The rotator cuff is a group of muscle that are responsible for guiding the shoulder and arm. It is really a sheet of muscle and when a part is torn, it must, by necessity, become slightly weaker. The bigger the tear, the more weakness the patient may notice.
Because it is a muscle, it also has the power to strengthen and so the remaining muscle, which is still attached, can get stronger and compensate for the torn part.
Unfortunately, the torn part can never heal itself spontaneously. It does not reattach.
When a patient has a torn rotator cuff, they notice two groups of complaints:
These notes should be read in conjunction with the explanatory notes on shoulder muscle pain. In that booklet, rotator cuff muscle pain was explained and the possibility that the rotator cuff can actually tear.
The rotator cuff is a group of muscle that are responsible for guiding the shoulder and arm. It is really a sheet of muscle and when a part is torn, it must, by necessity, become slightly weaker. The bigger the tear, the more weakness the patient may notice.
Because it is a muscle, it also has the power to strengthen and so the remaining muscle, which is still attached, can get stronger and compensate for the torn part.
Unfortunately, the torn part can never heal itself spontaneously. It does not reattach.
When a patient has a torn rotator cuff, they notice two groups of complaints:



